
Unveiling the Power of Your Smile
Your Smile: A Pathway to Happiness, Confidence, and Success In the picturesque city of Buford, GA, where the charm of Southern living meets the vibrancy
Read our valuable dental blog articles to boost your oral health & overall wellness.

Your Smile: A Pathway to Happiness, Confidence, and Success In the picturesque city of Buford, GA, where the charm of Southern living meets the vibrancy

Decoding the Tooth Extraction Cost: A Comprehensive Guide from Radiant Dental At Radiant Dental in Buford, GA, we understand that the prospect of a tooth
Root Canal Costs: A Comprehensive Guide by Radiant Dental in Buford, GA At Radiant Dental in Buford, GA, we understand that the prospect of a

Dermal Fillers Disco: Dance Your Way to a $10/unit Glow! Are you ready to dance your way to a radiant and youthful glow? At Radiant
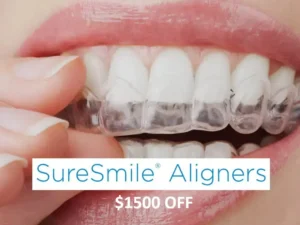
Get the Smile You’ve Always Dreamed of with $1500 Discount on Clear Aligners! Are you dreaming of a beautifully aligned smile without the hassle of

$99 Dental Emergency Special: Your Solution to Dental Crises When a dental emergency strikes, it can be a painful and stressful experience. Dental issues have
| Mon, Wed | 8:30 AM – 5:00 PM |
| Tue, Thurs | 11:00 AM – 7:00 PM |
| Saturday | 8:00 AM – 2:00 PM |